Learn how FP&A teams can transform cash flow forecasting with driver-based models, technology and collaboration to...

Introduction
Healthcare finance balances clinical needs with payer contracts and complex regulatory requirements, converting millions of patient encounters into consistent revenue and cash flow. It covers all aspects of commercial transactions, including budgeting, payment management, financial planning and debt recovery. Most FP&A teams currently use aggregated data, such as monthly charges, aging reports, and historical collection rates to forecast revenue, making manual adjustments for seasonal trends and known problems. While these methods are practical and familiar, they do not keep up with changing payment trends and operational disruptions, leaving finance teams to react to variances rather than anticipate them.
Today, healthcare revenue forecasts rely on past averages and delayed reports. In fact, roughly 1 in 5 medical claims are denied on first submission, and nearly 35 % of those denied claims are never resubmitted, resulting in substantial, preventable revenue loss for providers. Finance teams lack visibility into claim outcomes, that is, which claims will pay, which will be denied, or when cash will arrive. Key pieces of information are hidden within systems, leading to poor predictions, delayed actions, and lost opportunities to address revenue issues early.
This article explores how Artificial Intelligence (AI) can transform payment systems through an in-depth analysis of claim-level data, recognising payer patterns and using predictive modelling to anticipate outcomes before cash is realised. It helps FP&A teams see risks earlier, forecast cash more accurately, and move from explaining the past to shaping future financial results.
Challenges with the Traditional Approach
The biggest challenge with today’s healthcare FP&A approach is the limited insight into the various factors influencing revenue and cash flow schedules. Forecasts are built on summaries and averages based on historical data rather than specific claims or payor behaviours. Denials, appeals, and payment delays are often tracked outside core finance systems, making them hard to analyse at scale. Most of the time, issues are reported too late for timely action to rectify them. As a result, finance teams devote too much time to resolving forecast errors rather than preventing them, hindering their capacity for swift, strategic planning.
Methodology: Turning Healthcare Revenue into FP&A Intelligence
Transforming revenue into a strategic FP&A asset requires a shift from periodic reporting to continuous, data-driven insight. The methodology is less about adopting a single AI tool and more about redesigning how revenue data flows into planning and forecasting. Below are high-level steps:
Consolidate Revenue Data at the Claim Level
To get meaningful insights, we need to start bringing data from billing systems, remittance files, claim status feeds, payer portals, and appeal workflows. The goal is a single, normalised view of each claim, from service delivery to the final cash outcome, rather than disconnected summaries.Convert Operational Data into Analyzable Signals
Unstructured denial reasons, payer messages, complete claim information, including all services included in each claim, and appeal notes are translated into consistent categories. Key attributes such as payer behaviour, service type, timing patterns, and historical outcomes are standardised to enable reliable analysis.Apply AI to Predict Claim Outcomes and Cash Timing
With enough data, we can train Machine Learning models, and these models can be used to assess the probability of payment, denial, appeal success, and expected collection timing for each claim. Instead of assuming average collection rates, FP&A gains visibility into likely cash distributions across the receivables portfolio. Real-world adoption of AI in revenue cycle processes has been linked to 30-40 % reductions in denial rates and 30–50 % cuts in administrative costs, while accelerating claims turnaround by up to 60 % compared with traditional workflows.Integrate Predictive Outputs into FP&A Forecasts
Forecasts are updated using probabilistic cash flows rather than static assumptions. Revenue projections reflect real payer behaviour, denial risk, and operational delays, improving forecast accuracy and scenario planning.Establish Continuous Monitoring and Feedback Loops
As new claim activity and payer responses occur, models are refreshed and forecasts adjust in near real time. Variances become early warning signals, enabling finance teams to intervene before revenue leakage materialises.Embed Insights into Strategic Decision-Making
FP&A uses this intelligence to inform working capital planning, payer negotiations, service line strategy, and investment decisions. Revenue cycle performance is no longer just operational data; it becomes a core input into enterprise financial strategy.
Figure 1 illustrates how claim-level revenue data flows from operational systems into FP&A forecasting and decision-making, highlighting the shift from periodic, average-based planning to continuous, signal-driven revenue intelligence.
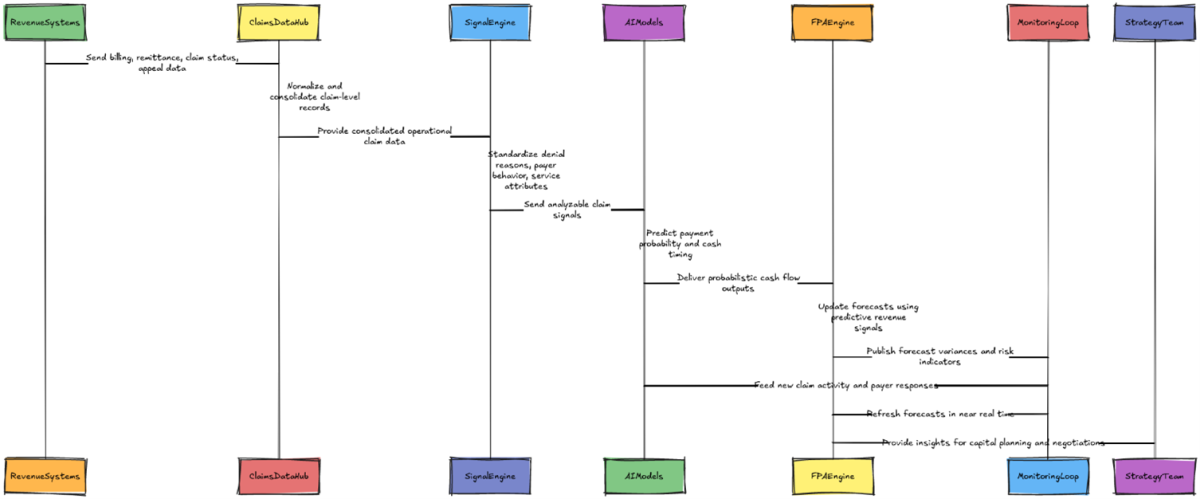
Figure 1: Implementation Steps Sequence Diagram
Case Study: Embedding AI into Healthcare FP&A Forecasting
A large integrated healthcare organisation operating multiple dental speciality clinics relied on a traditional FP&A revenue model built around payer mix, historical collection percentages, and average days in accounts receivable. Revenue cycle teams managed denials and appeals separately using operational dashboards and manual worklists. FP&A received only summarised monthly outputs, limiting visibility into timing risk and payer behaviour.
The organisation introduced an AI-driven revenue intelligence layer between revenue cycle systems and FP&A. Claims data from billing platforms, remittance files, claim status feeds, and payer portals were consolidated into a normalised data model. Natural language processing was used to standardise the reasons for denials in payer messages and appeal letters. Machine learning models classified claims by likelihood of first-pass payment, appeal success, and expected collection timing.
These outputs are fed directly into FP&A cash flow and revenue forecasting models. Instead of applying flat collection assumptions, FP&A forecasts reflected different cash timing scenarios based on claim risk categories. Forecast updates shifted from monthly to rolling, event-driven updates as claims progressed through the revenue cycle.
Over time, FP&A began using these insights to support working capital planning, evaluate payer contract performance, and escalate operational issues earlier. Revenue forecasting evolved from historical estimation to a forward-looking, intelligence-driven process aligned with real payer behaviour.
Practical Challenges and Recommendations for Healthcare FP&A Leaders
Challenges:
FP&A leaders face real obstacles when adopting AI-driven revenue intelligence. Revenue data is fragmented across billing systems, payer portals, and manual workflows. Denial reasons are inconsistent and often unstructured. Finance teams may be uncomfortable with probabilistic forecasts, and IT teams are stretched with competing priorities. Measuring ROI upfront is difficult, slowing executive buy-in.
Recommendations:
Start small and be practical. Focus on high-impact use cases, such as denial risk or cash timing. Invest early in data quality and cross-functional ownership. Educate FP&A teams on probability-based forecasting. Treat revenue intelligence as long-term infrastructure, not a one-time analytics project.
Future outlook:
Looking ahead, AI is poised to reshape how healthcare FP&A teams forecast and manage revenue fundamentally. Advances in real-time data integration, natural language processing, and explainable AI will make predictive insights more accurate, transparent, and actionable. FP&A leaders will shift further away from descriptive reporting toward scenario modelling, automated risk alerts, and strategic planning informed by payer behaviour patterns. As interoperability improves, cross-organisational benchmarking and shared learning will become possible. Over time, revenue cycle intelligence will integrate with enterprise performance management platforms, turning operational signals into strategic foresight and enabling healthcare finance to drive both financial resilience and organisational growth.
Conclusion
Healthcare revenue forecasting is at an inflexion point. Traditional average-based and lagging models are no longer sufficient in an environment shaped by complex payer behaviour, rising denials, and operational volatility. AI offers FP&A leaders a practical path to convert fragmented revenue cycle data into forward-looking financial intelligence. When revenue is treated as a dynamic signal rather than a historical outcome, forecasts become more reliable, decisions timelier, and finance more strategic. Organisations that invest early in revenue intelligence will gain lasting advantages in cash visibility, planning confidence, and financial resilience. More importantly, the role of FP&A itself expands from explaining revenue variance after the fact to actively shaping revenue predictability and response strategies.
From a leadership perspective, this shift calls for FP&A teams to own rolling, probability-based revenue forecasts, clearly separate performance targets from unbiased forecast views, and lead forward-looking conversations around revenue risk and cash timing. AI-enabled revenue intelligence thus becomes not just an analytical capability, but a core leadership instrument for enterprise planning and performance management.
References
Subscribe to
FP&A Trends Digest

We will regularly update you on the latest trends and developments in FP&A. Take the opportunity to have articles written by finance thought leaders delivered directly to your inbox; watch compelling webinars; connect with like-minded professionals; and become a part of our global community.







